Home & Community
Rehabilitation Wherever Life Happens
Rehab Without Walls® home and community rehab blends evidence-based therapies with creative uses of the patient’s surroundings – whether at home, school, work, or in their own community.
Providing rehab therapy in a home and community environment offers a huge advantage in treatment. Addressing goals and barriers in real-life settings can increase motivation, lead to more durable outcomes, and reduce the risk of injuries that could lead to rehospitalization.
For over 30-plus years, we’ve served thousands with our home and community rehab programs – and produced proven results that have been published in numerous peer-reviewed medical journals.
When is home and community neuro therapy the right fit?
Home and community neuro therapy is best suited for adults and children who:
- Are medically stable enough to go home.
- Have appropriate support for safe transition to home and/or have limited access to transportation to facility-based programs.
- Will experience a clinical advantage, such as functional goals requiring practice in their own home or community setting.
Our neuro therapy programs are covered by some commercial health insurance and workers’ compensation plans. Medicare does not cover home and community-based rehabilitation.
Typical
Home Health
rehab model
- Medical Model
- Medicare certification requiring homebound status
- Intermittent therapy visits 3-6 hours/week
Typical Home Health
vs
RWW Home and Community Rehab
Home & Community
Neuro Rehabilitation
Advantage
- Rehabilitation Model
- Homebound status NOT a barrier to care
- Intense rehab program = 10-25 hours/week with neuro skilled clinicians
Our Approach
It’s quite simply who we are, we believe in removing the walls associated with neuro rehab – including physical, emotional, and environmental – and focusing on:
- Teaching relevant skills in the individual’s environment as opposed to a staged setting.
- Going beyond personal care to real-life experiences like navigating the kitchen, the bathroom, the grocery store and workplace.
- Building the individual’s personal goals into the therapy plan.
Through this program, instead of just learning to prepare a meal, individuals will learn to shop in their local grocery store and use their own kitchen. Rather than simply focusing on grooming skills, they will learn to navigate their own bathrooms safely.
A comprehensive evaluation is conducted by an interdisciplinary team upon admission to assess for and identify safety issues in both the home and local community.
Evaluation of accessibility, emergency preparedness including ability to exit home in event of an emergency, fall risk, equipment needs/ appropriateness of existing equipment, caregiver support and community resource needs are some of the items evaluated. Our evaluation includes understanding our patients cultural beliefs, learning needs, telecommunication abilities and life stressors as these our pivotal to successful treatment and patient outcomes.
A home safety evaluation is an integral part of our approach. Before therapy begins, we’ll conduct a one- to two-hour inspection focused on:
- Fire hazards.
- ADA specifications for wheelchair-bound individuals (ramps, door widths, etc.).
- Whether an individual would be able to exit the house safely.
- Modifications in the bedroom, bathroom and kitchen that could help the individual be more independent.
- Which surfaces, furniture and rugs might be hazardous or act as impediments.
- Whether the stairs can be navigated safely.
- Which adaptive equipment currently in use might need to be upgraded.
- If the outside terrain is safe and navigable.
Care Team
Our expert team will create a individualized therapy plan for each patient in the home and community rehab program that incorporates elements of the individual’s home into therapy. For example, range of motion can come through daily chores; eye-hand coordination from working on the computer; organizational skills from meal planning and grocery shopping.
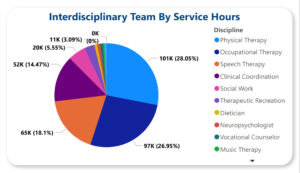
The home and community rehab care teams is overseen by a physician and led by a clinical coordinator. The clinical coordinator pulls together the right team, ensures that there are no gaps or overlaps in services, facilitates communication, and leads frequent team meetings that include our patient, therapists, patient’s physician and their families as well as other external stakeholders such as case managers, care givers and specialized medical equipment experts.
Our home and community care team may include experts from the following therapy disciplines:
- Physical, Occupational and Speech Therapy
- Recreational Therapy
- Psychology & Neuropsychology
- Dietitian
- Licensed Clinical Social Worker and Clinical Counseling
- Clinical Coordination
- Music Therapy
- Vocational Therapy
- Special Education Tutors
Home & Community Program Outcomes
2024 Home and Community Rehabilitation Outcomes
Rehab Without Walls® home and community rehab blends evidence-based therapies with creative uses of the patient’s own surroundings – whether at home, school, work, or in their own community.
Addressing goals and barriers in real-life settings can increase motivation, lead to more durable outcomes and reduce the risk of injuries that could lead to rehospitalization.
Outcomes are important indicators of a program’s success. At Rehab Without Walls, we use outcomes to measure our effectiveness in helping people improve their quality of life and return to independent living after an injury or illness.
2024 Patients Served

Mayo Portland Adaptive Inventory (MPAI-4) and Supervision Rating Scale (SRS)
The MPAI-4 assesses how well a person is doing after an acquired brain injury. It measures the areas of ability (physical and cognitive skills), adjustment (anxiety and depression) and participation (social interaction and self-cares). The lower the score, the higher the level of independence. Our goal is to make at least a 5-point change from admission to discharge.
And the SRS describes someone’s ability to be home alone without assistance. While any level of improvement in independence can be meaningful to a patient and their support system, our goal is to help our patients be home alone for 8 hours or more by discharge. We compare scores taken at admission, discharge, 3 months after discharge and 1 year after discharge.

MPAI Chronicity
MPAI Chronicity shows improvement across length of time from when the injury or illness happened and when the patient was admitted to Rehab Without Walls. This can show the ongoing success of the rehabilitation process, even years after the injury.
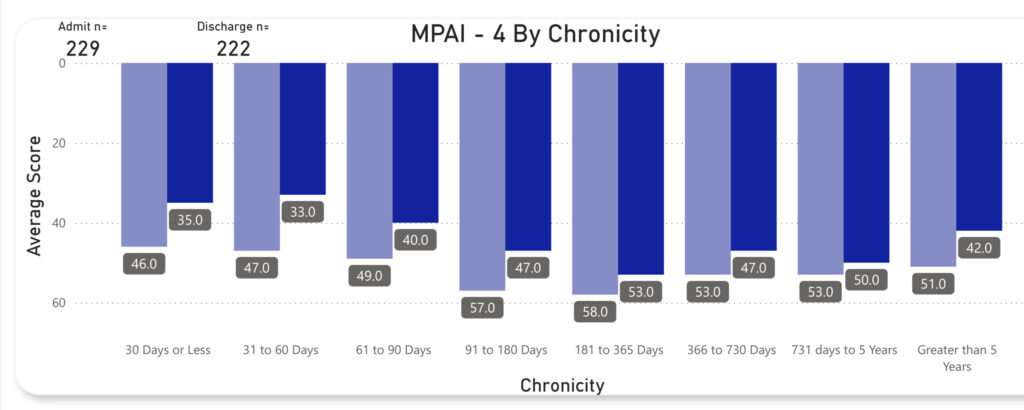
The earlier RWW Home and Community begins services from injury the greater the results. RWW continues to see improvement greater than 5 years post injury.


Spinal Cord Injury Program Outcomes
2024 Outcomes in the Home and Community Spinal Cord Injury Specialty Program-
Outcomes are important indicators of a program’s success. At Rehab Without Walls, we use outcomes to measure our effectiveness in helping people improve their quality of life and achieve maximum level of independence after spinal cord injury or disease.

Supervision Rating Scale (SRS) describes someone’s ability to be home alone without assistance. While any level of improvement in independence can be meaningful to a patient and their support system, our goal is to help our patients be home alone for 8 hours or more by discharge. We compare scores taken at admission, discharge, 3 months after discharge and 1 year after discharge.

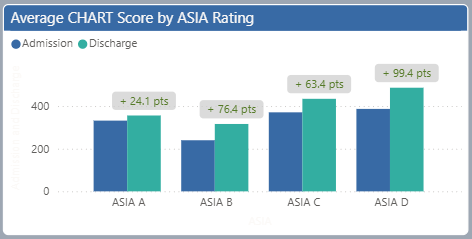
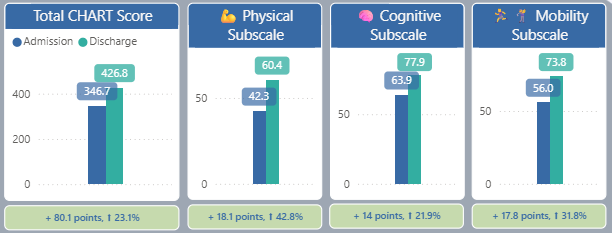
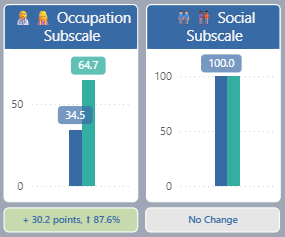
Craig Handicap Assessment & Reporting Technique (CHART) measures the total impact of spinal cord dysfunction on return to life roles. This includes physical independence (how much help is needed for everyday activities like getting out of bed, getting dressed, using the restroom, and making simple meals), mobility (ability to access both home and community environments, including getting out of bed, getting out of the house and staying away for the night), occupation (return to productive activity including work, school and homemaking) and social interaction (participating in and maintaining relationships). A higher score indicates a higher level of independence. Scores are compared at admission, discharge, 3 months after discharge and 1 year after discharge.