Home
Home

News Articles
PATIENT STORY: PATIENT CENTERED REHABILITATION
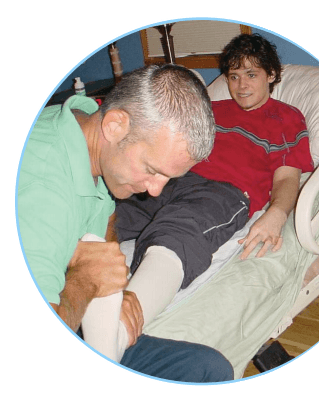
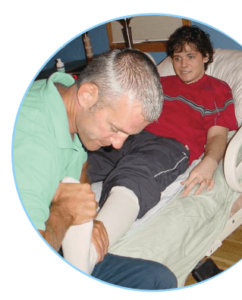
Although we say Rehab Without Walls® NeuroSolutions provides neurorehabilitation, in truth we offer a more encompassing kind of treatment – something we like to call patient-centered rehabilitation.
What does this mean? In essence, it means that we focus on obtaining meaningful results that allow the patients to live as independently as possible with a high quality of life. For example, we want to be sure that a mother not only regains muscle strength and range of motion, but is able to carry her child in her arms. Or that a patient not only restores cognitive skills, but is able to use them purposefully at work or school.
In order to create these real-life, meaningful results, we know we need to treat more than the patient’s physical symptoms. We need to understand the core of his or her life, work with the family and support systems, connect with community resources, tap into the patient’s internal motivation, recognize emotional issues that may impede progress, identify subtle barriers and find innovative ways to remove them, and help patients embrace their recovery within the context of who they now are and what they are capable of doing.
To best illustrate how this approach works, we’ve zeroed in on a single case at the Rehab Without Walls NeuroSolutions Michigan location and spoken with several treatment team members, including the patient’s family. By focusing on all the details, the big picture – our whole person approach to rehabilitation – becomes even clearer.
As a 20-year-old at Michigan State University, Sam Howell was the top biochemical student in the world. In fact, during his freshman year, he was invited to assist a Harvard University professor in a research project on lymphomatoid papulosis. Less than a month after his return to Michigan, however, he was in a such a severe motor vehicle accident that his parents were told that he had just a 2 percent chance of survival. Sam spent 2½ months in a coma, emerging from it severely impaired – unable to speak, walk or care for himself. Sam’s family rallied around him, determined that not only would he recover, but that he would once again lead a full life that tapped into his considerable intellectual gifts.
Looking for the right team
Sam’s mother Maureen, an ICU nurse, contacted 25 different health care facilities and agencies looking for the right rehabilitation team for her son. “I wanted people who were comfortable and experienced with head injuries. It was key for Sam to undergo rehabilitation at home because of his reduced stamina due to pituitary failure with secondary adrenal gland insufficiency,” explains Maureen. “As soon as I met with Rehab Without Walls, I knew it was the right fit.” With Rehab Without Walls, the family began assembling the treatment team. Maureen left her job to serve as the 24-hour RN. She also, with the agreement of their insurance company, brought on their own speech language pathologist, Randi Michael, SLP, from a local facility, because her skills best matched Sam’s needs. “That was not a problem,” says Clinical Coordinator Steven Mandley, who also served as PT on the case, “because what’s best for the patient is what’s best for us.”
Understanding the patient’s unique qualities
From their first meeting with the family, the treatment team members realized that they were not dealing with an ordinary head injury patient. “Typically, there is some, if not significant, cognitive impairment,” says Rachel Barrett, the team’s occupational therapist, “but in Sam’s case, his intellect had not been affected at all. Here we had a patient and family that were highly educated and highly motivated. We had to adjust our approach and techniques to reflect this.”
As the team got to know Sam, they began to understand how much his personality could impact treatment. “He was very strong willed, competitive and goal oriented. At age two and a half, he had taught himself to read. Plus, with his scientific background, he had a strong sense of perseverance, and an understanding that you need to take baby steps to get to the bigger goal,” Barrett says. “So we co-opted this idea, and framed his treatment in those terms.”
In addition, she adds, “there was so much love in that house. This, in turn, supported the treatment tremendously. The family was always open to trying something new. They came at a problem from all angles, they always followed through on treatment exercises and techniques, and they contributed their own skills to the rehabilitation process.” For example, Sam’s two sisters, both teachers, set up a handwriting program for him. All the adult family members, including brothers-in-law, received training from the Rehab Without Walls team so they could help with assists. And one of the brothers-in-law, a carpenter, built practice stairs and a custom standing frame so Sam could stand longer with less assistance.
Setting goals
Sam’s mandate was to be independent, which included returning to school, sports and his research activities. The challenge was finding ways to bridge the gap between Sam’s intellectual acuity and extreme motivation and his physical deficits without letting him become discouraged with the pace of progress. “He initially used a spellboard the first few months so he could communicate while the speech therapist worked with him on his vocalization,” says Mandley. “We also let him learn through experience, which helped him deal with his frustration in not reaching goals sooner. For example, he knew how much he was practicing and thought he could do more with less assistance, so we let him try. When he lost his balance, Sam had the necessary proof to understand that he did indeed need more assistance. We framed as much as we could scientifically and empirically because that made sense to him.”
Regaining speech was one of the key goals, and the trickiest to reach because even when Sam was speaking, understanding him was difficult. “This was due to extreme muscle weakness, including poor jaw control and impaired range of motion with the tongue,” explains Speech Language Pathologist Randi Michael. “We later discovered he had velopharyngeal insufficiency, which basically meant that it took extraordinary respiratory effort to speak because the muscles didn’t close off on certain sounds and he would lose air out of his nose.” Some of Sam’s doctors strongly advised that he get a computerized voice machine, but his parents disagreed entirely. Michael implemented an oral motor home exercise program and re-taught Sam each sound (phoneme), one phoneme at a time. This technique worked remarkably well and at present, Sam’s family can understand his speech 90 to 95 percent of the time.
There were also problems with swallowing. In response, Michael obtained certification in Vital Stim therapy, which uses small electrical currents to stimulate the muscles responsible for swallowing, and is used in conjunction with therapists who help patients “re-educate” their muscles. She also taught him compensatory safe swallow strategies. Again, progress was remarkable, and Sam was able to attain his nutritional needs via oral intake of mechanical soft solids and nectar thick liquids.
Co-treatments are key
Throughout the entire treatment process, therapists and family members teamed up to reinforce the teaching from the individual disciplines. For example, the speech therapist taught the PT what to listen for and what to correct while Sam was speaking during his exercise sessions. As a reinforcement to both teachings, the PT would write down all the steps of an exercise and ask Sam to verbalize them. During initial gait training sessions, the PT worked with Sam’s leg coordination while the OT addressed proper trunk alignment and body dynamics. Speech therapy would be conducted while Sam was standing so he could also practice proper posture. Family members would review speech exercises with Sam in the car, and so on. “The team effort is so important,” says Barrett, “because we work off of each other to ensure that nothing slips through the cracks. If one of us misses something, the other will catch it. We also continually brainstorm together to find new solutions to problems as they emerge.”
Looking at subtle but important interventions
High on the list of priorities for Sam, his family and the team, was to minimize the appearance of disability. Not out of vanity, but because it was important that people see Sam and his intellect first – not his deficits. “This was a key piece for Sam to return to his world,” says Michael, “and an important part of his quality of life. We didn’t want to settle for ‘just good enough.’ It wasn’t good enough that he could just speak; we wanted him to speak articulately so that everyone could clearly understand him. It wasn’t good enough that he could move, we wanted him to move without tics or distracting mannerisms.” Adds Barrett, “We’re looking at the quality of his movement and how it transfers to the big picture. We continually ask ourselves ‘how normal does he look in public?’”
Another Rehab Without Walls NeuroSolutions priority is the emotional stability of the family. In this case, the family was extraordinary but the stress of dealing with their medically fragile son and the day-to-day challenges of his treatment took its toll. The team brought a psychologist on board so the family could learn new coping skills. “Supporting the patient and family during these times cannot be underestimated,” says Mandley. “The stresses on them can be crushing, and the usual ways in which they deal with a crisis may simply not be enough. The family’s ability to support the patient can be the foundation for rehabilitation.”
Driving each part toward the whole
In this case, progress has continued on an upward trajectory, with no plateaus. More typically, patients will reach their goals and start to plateau. At that point, the rehabilitative gains become minimal and the team begins to taper treatment toward discharge. Sam, however, has continued to achieve functional goals and move on to new ones, so the team has remained in place. “We’ve followed the lead of Sam and his family and have not set restrictions or limitations on him – despite the poor prognosis his doctors offered. There’s no reason why he can’t go back to school and become gainfully employed,” says Michael. “Each of us both together and apart is doing everything we can to make that happen.”
Editor’s note:
Sam and his family continue to advocate for people who have had traumatic brain injuries. Read more in these articles from MLive Media Group:
Michigan man, who beat the odds after car crash, fights against no-fault insurance reform